Two new breakthrough treatments brings fresh possibilities for those living with chronic plaque psoriasis.... Read more >
Psoriasis: why starting (and staying on) treatment matters
Psoriasis: why starting (and staying on) treatment matters
Psoriasis isn’t only skin-deep. Finding the right treatment can help you better manage your psoriasis from the inside out.
Published 14 June 2023

Normally, it takes about a month for the body to grow new skin cells, but when you’re living with psoriasis, a glitch in the immune system turbocharges the process, launching an inflammatory blitz that shortens it to mere days. Result? The older skin cells can’t shed fast enough, so they pile up, creating scaly patches (called plaques) that may appear on any area of the body, from the scalp and the face to the hands, nails and feet — and everywhere in between.
What many people don’t realise about psoriasis — including those who have it — is that it’s not just the skin that’s affected. Researchers suspect that the same inflammation that wreaks havoc on the skin may stealthily go to work on other organs and systems of the body, causing problems elsewhere.
Here’s a closer look at how psoriasis goes beyond your skin — and how finding the right treatment and staying the course can help you better manage psoriasis from the inside out.
Psoriasis: more than skin deep
One in three people with psoriasis goes on to develop psoriatic arthritis, a disease that causes pain, stiffness and swelling in and around the joints and can lead to permanent joint damage.
Studies show that people with psoriasis are also more likely to have one or more of the following conditions:
- Chronic obstructive pulmonary disease
- Inflammatory bowel disease
- Obesity
- Polycystic ovary disease
- Sleep apnoea
- Uveitis
And there’s also a surprisingly strong link between psoriasis and diabetes, elevated cholesterol levels and high blood pressure. All of these increase your risk of cardiovascular disease and make you vulnerable to heart attack and stroke, explains Frank Wang, MD, William B Taylor Endowed Professor of Clinical Dermatology, University of Michigan, Ann Arbor. “There’s probably some systemic inflammation that damages blood vessels and sets the stage for heart disease.”
For those reasons, Allison Ruff, MD, MHPE, a primary care physician at the University of Michigan Health and clinical associate professor at the University of Michigan Medical School, is adamant that people with psoriasis follow up with their GPs regularly. “While dermatologists are experts in the skin, GPs are best suited to evaluate people with psoriasis for metabolic conditions, such as diabetes and high blood pressure; some cancers; and mental health concerns, such as anxiety and depression.”
Mona Gohara, MD, Associate Clinical Professor of Dermatology at Yale School of Medicine in New Haven, Connecticut, agrees. “Gone are the days when somebody comes in the office and we give them a cream and have them walk out the door when they have psoriasis.”
How psoriasis treatment can help stave off complications
Today, there are more options than ever for managing psoriasis, so if you’re willing to try different strategies (hang in there, it may take some trial and error), odds are you’ll find a treatment that works for you.
What’s more, effective treatment won’t just clear your skin but may also help lower your chances of developing associated conditions. For example, says Dr Wang, “There is emerging evidence that using a systemic agent, such as an oral anti-inflammatory or a biologic, can help your cardiovascular risk as well. And some of the same medications used to treat the skin will also improve the joints in people who have psoriatic arthritis.”
One factor your dermatologist will consider when determining your treatment plan is the severity of your disease. If less than three per cent of your skin is covered, your case is considered mild; from three per cent to 10 per cent, moderate; and more than 10 per cent, severe. Dermatologists also use tools like the Psoriasis Area and Severity Index (PASI), which look at criteria such as the thickness and scaliness of your plaques in addition to the surface area they cover.
Another important factor your dermatologist will consider is how you feel about your psoriasis. Even a textbook “mild” case can cause a person to feel uncomfortable, embarrassed or otherwise distressed and should be treated as aggressively as the patient desires.
Understanding your psoriasis treatment options
After evaluating your psoriasis and getting your input, your dermatologist may discuss different ways for you to find relief, including home remedies such as soothing baths, sound sleep, using the right skin products and more. In addition, they will review the following treatment methods, and together you can decide on the approach that makes sense for you.
Topical treatments
As the name suggests, these are creams and ointments that help ease inflammation, swelling and itching when applied to the skin.
Over-the-counter options include:
- Hydrocortisone cream which soothes redness, swelling and inflammation.
- Numbing/anti-itch creams.
- Coal tar treatments, which relieve inflammation and slow the growth of skin cells.
- Medicated shampoos for scalp psoriasis.
- Products that contain salicylic acid (creams, shampoos and lotions), which help the body shed excess skin.
Prescription topicals include:
- Corticosteroids which relieve inflammation and help shed excess skin.
- Vitamin D analogues that slow the growth of skin cells.
- Calcineurin inhibitors which block a chemical that triggers inflammation.
- Retinoids, a form of vitamin A that can slow skin cell growth, reduce dryness and promote shedding.
- Anthralin, a thick, pasty cream that was one of the original psoriasis treatments.
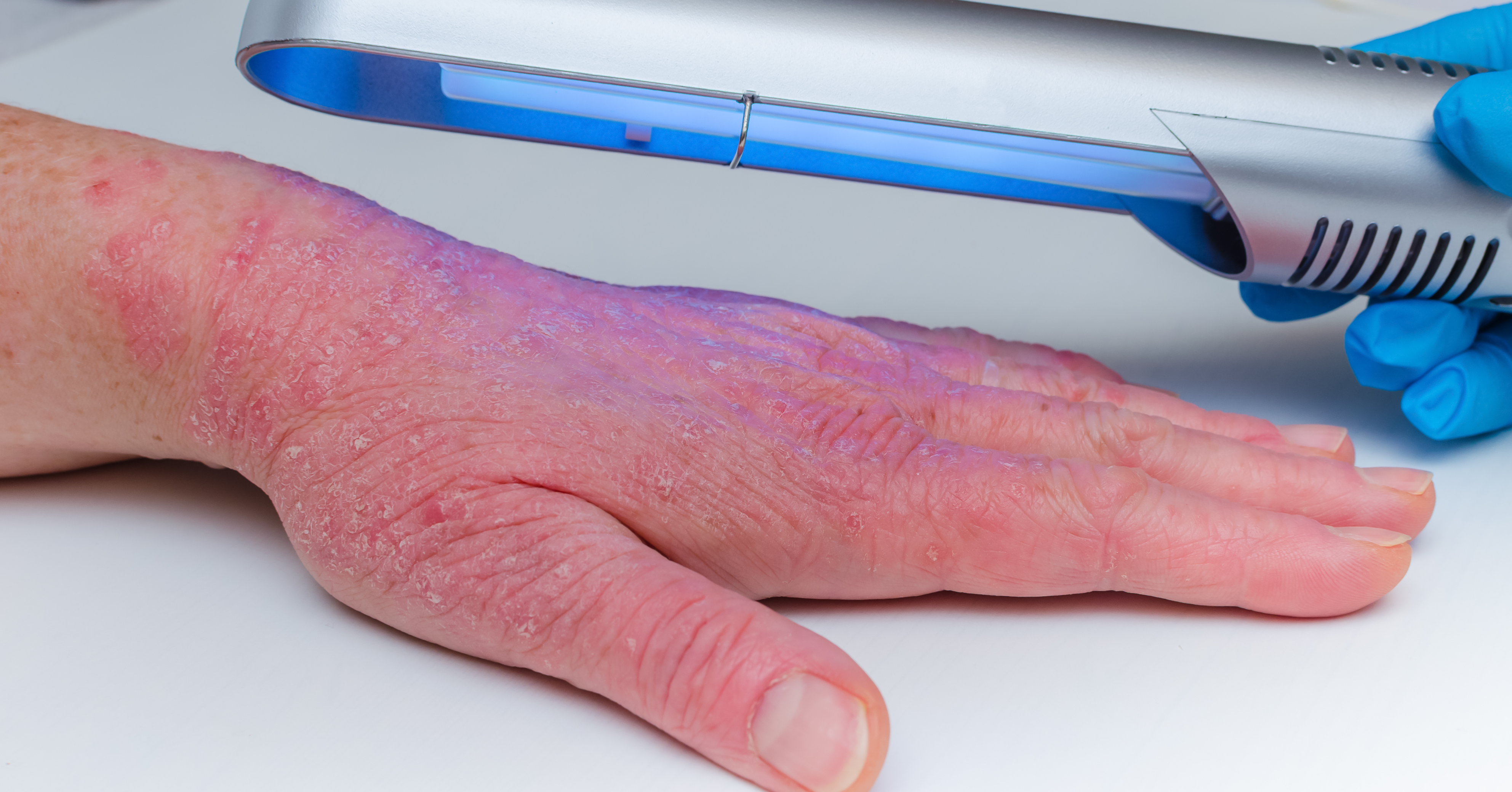
Ultraviolet light therapy
Also called phototherapy, this treatment involves exposing your skin to ultraviolet light to help slow the growth of skin cells and help clear plaques. Your dermatologist will determine the number of sessions you need. Light therapy is available in Australia through dermatology clinics and is subsidised by Medicare.
Body-wide (systemic) medications
When psoriasis does not get better with the use of topicals or phototherapy, doctors may suggest moving to a medication that works throughout the body, also known as a systemic treatment.
The first option they’ll usually recommend is a disease-modifying antirheumatic drug (DMARD) like methotrexate or cyclosporine. Taken orally, these medications not only help relieve symptoms but may also help fend off or stop the progression of psoriatic arthritis. Other oral options include PDE4 inhibitors, newer drugs that target molecules inside immune cells to help curb the inflammatory cycle behind psoriasis.
Biologics, given by injection or infusion, are another type of systemic treatment. Made in a laboratory from living cells, biologics work by blocking specific parts of the immune system that cause the overgrowth of skin cells. For example, some biologics are IL-12, Il 12/23 IL-17 or IL-23 inhibitors while others are TNF-inhibitors, and many other pathways are currently being studied.
Getting psoriasis under control is life-changing
In addition to skin symptoms and the related diseases discussed above, psoriasis often takes another toll. “Many patients with psoriasis can also have psychiatric and emotional concerns, such as depression and anxiety, substance abuse and self-harming behaviours brought on by the stigma associated with the disease,” says Dr Wang. In fact, researchers refer to it as a “psychosocial skin disease” for the impact it can have on a person’s self-esteem, leaving many people in the psoriasis community feeling lonely and isolated.
This impact is often unknown to the general public and even medical professionals. According to Mark Lebwohl, MD, Dean for Clinical Therapeutics and a Professor of Dermatology at Mt Sinai Hospital in New York City, his Canadian colleague conducted an experiment with first-year medical students to show them the stigma attached to psoriasis. He had them paint tattoos depicting areas of psoriasis on the students’ visible skin. “Before they started the study, they thought that psoriasis was a trivial disease,” he says, “Then they walked around with those tattoos for just a few days. The impact on the way other people treated them was so striking that, to them, it suddenly became a serious disease.” Read about how to cope when people stare at your psoriasis.
When a person finds a treatment that works, it can turn their world around. “My medications gave me my life back,” says Ashley K, who had six or seven medications fail her before finding a therapy that worked for her psoriasis and psoriatic arthritis. “I could cook meals, do laundry, clean, run errands. I wasn’t tired all the time and I was happy that I could be of value and contribute to my family … and go to school and do advocacy work.”
The right treatment restored Reena Ruparelia’s confidence. She waited 26 years for plaque-free skin. “I wanted to express myself through clothing and jewellery, but I didn’t want people to look at me and feel disgusted so I wore things that would let me blend into the background,” says the Toronto-based mindful living guide. Then, last summer, she started a new treatment, and the anxiety and self-doubt lifted. “My skin is clear for the first time since I was diagnosed.”
Reena now loves to go dancing on weekends in her favourite gold dress. I finally feel “at peace with myself and being there with myself,” says the 41-year-old, who shares her psoriasis journey at Reenarup.com.
Diane T can certainly relate. “When my skin started clearing up, I was over the moon. I remember telling my husband, ‘I want to go to the store to buy a blouse — a short-sleeved blouse. I had never bought a short-sleeved blouse in my whole life.”
Found something that works? Stay the course
“There’s no cure for psoriasis,” reminds Dr Wang. So, if you find a treatment that works for you, it’s a good idea to stick with it, unless you are experiencing intolerable side effects.
In this case, you’ll need to understand your own threshold as well as work with your healthcare team to see if you can make any adjustments or just switch therapies altogether.
“There’s a point where you know your body and can say, okay, maybe I need to push through these for the first couple of weeks and get through those side effects. And all medications can have side effects,” says Ashley K. “But if you’re two months out, and your doctor is still telling you to stay on it, I would 100 per cent try to find a new doctor. Everybody is so different, so you just have to listen to your own rhythm and go from there.”
Of course, your journey is yours alone. But to make the smartest moves, it’s best to discuss all decisions with your psoriasis care team. They can help you understand the pros and the cons and how they may impact you, your skin and your overall health — both now and in the future.
If this article has raised feelings that concern you, visit the Lifeline website or call 13 11 14.
This information should never replace the information and advice from your treating doctors. It is meant to inform the discussion that you have with healthcare professionals, as well as others who play a role in your care and well-being.
This article has been adapted, with permission, from a corresponding article by Maria Lissandrello on the CreakyJoints US website. Some content may have been changed to suit our Australian audience.
Harvard Health Publishing: Diseases and Conditions https://www.health.harvard.edu/diseases-and-conditions/taming-the-chronic-inflammation-of-psoriasis
Van Hal T, et al, Discovery of Arthritis in Psoriasis Patients for Early Rheumatological Referral (DAPPER): Protocol for a Longitudinal Observational Study, JMIR Res Protoc 2021;10(11):e31647, URL: https://www.researchprotocols.org/2021/11/e31647, DOI: 10.2196/31647
Oliveira Mde F, Rocha Bde O, Duarte GV. Psoriasis: classical and emerging comorbidities. An Bras Dermatol. 2015 Jan-Feb;90(1):9-20. doi: 10.1590/abd1806-4841.20153038. PMID: 25672294; PMCID: PMC4323693. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4323693/
Tsai YC, Tsai TF. Anti-interleukin and interleukin therapies for psoriasis: current evidence and clinical usefulness. Ther Adv Musculoskelet Dis. 2017 Nov;9(11):277-294. doi: 10.1177/1759720X17735756. Epub 2017 Nov 6. PMID: 29344110; PMCID: PMC5764033. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5764033/
Choudhary S, et al. Psoriasis and cardiovascular disorders: association or epiphenomenon? Meta-analysis of observational studies. 3 Biotech. 2020 Mar;10(3):104. doi: 10.1007/s13205-020-2089-6. Epub 2020 Feb 7. PMID: 32099745; PMCID: PMC7007463. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7007463/
Ferreira BI, Abreu JL, Reis JP, Figueiredo AM. Psoriasis and Associated Psychiatric Disorders: A Systematic Review on Etiopathogenesis and Clinical Correlation. J Clin Aesthet Dermatol. 2016 Jun;9(6):36-43. Epub 2016 Jun 1. PMID: 27386050; PMCID: PMC4928455. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4928455/
Further reading
- Psoriasis, psoriatic arthritis and hair loss: its causes and what to do about it
- My journey with psoriasis, psoriatic arthritis and peer support
- Growing up with psoriasis: Mother and daughter share their stories
- How to build your psoriasis healthcare team
- Government Support for People with Chronic Conditions





This Post Has 0 Comments